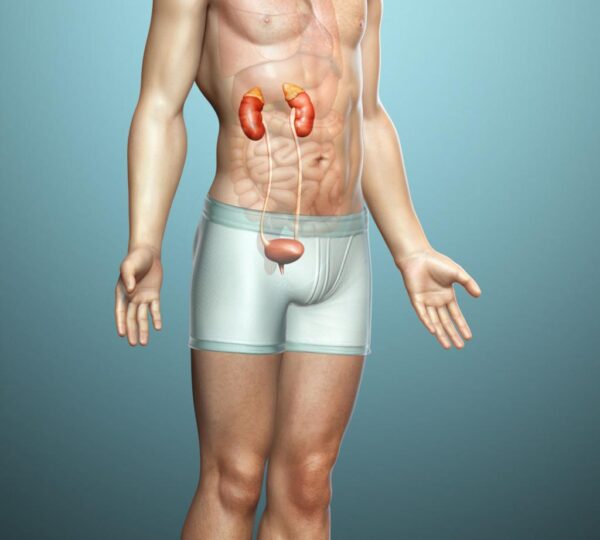
The kidneys are remarkable organs, working quietly behind the scenes to maintain balance within the body. Despite their small size, they filter roughly 50 gallons of blood daily, ensuring toxins are removed and essential nutrients preserved.
Their silent nature often misleads people into underestimating their importance. Unlike the heart or lungs, kidneys rarely send immediate warning signals, allowing damage to progress over months or even years before noticeable symptoms appear.
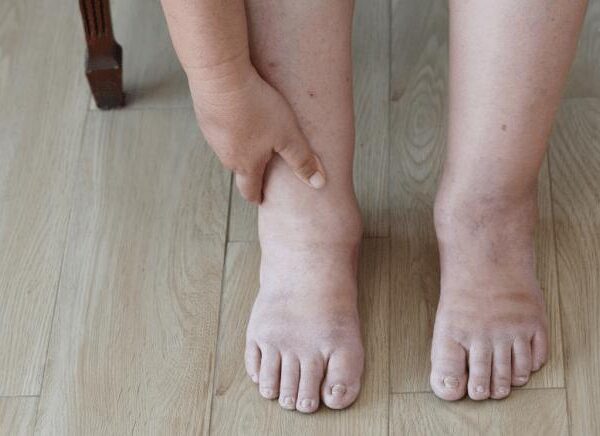
This delayed onset is one reason kidney disease can be particularly dangerous. By the time fatigue, swelling, or changes in urination manifest, significant loss of kidney function may already have occurred, limiting treatment options.
Kidneys are responsible for far more than simply removing waste. They regulate blood pressure through hormone control, balance electrolytes like sodium and potassium, and produce erythropoietin, which signals bone marrow to create red blood cells.
Because these organs operate continuously, they compensate for minor damage with extraordinary resilience. Even with partial dysfunction, they often maintain near-normal function, masking the effects of ongoing strain and delaying detection until advanced stages.
Modern lifestyles place unrecognized stress on kidney health. High-sodium diets, excessive sugar, and processed foods increase the workload on these organs, forcing them to manage fluid and mineral imbalances under chronic metabolic pressure.
Sedentary habits contribute as well. Physical inactivity slows circulation, reduces metabolic efficiency, and can promote obesity, diabetes, or hypertension—all major risk factors for kidney disease and other organ dysfunction.
Chronic stress exerts a subtler influence, triggering hormonal cascades that elevate blood pressure, increase inflammation, and gradually strain the kidneys’ delicate filtration system. Over time, this persistent pressure accumulates silently.
Even commonly used medications can be risky when taken excessively or without medical guidance. Pain relievers like NSAIDs, certain antibiotics, and over-the-counter supplements may contribute to kidney damage if repeated over weeks or months.
Hydration is a cornerstone of kidney preservation. Water facilitates filtration, helps maintain electrolyte balance, and reduces the risk of kidney stones. Inadequate fluid intake silently increases concentration of toxins and crystallization risk.
Early kidney damage is often asymptomatic. Subtle signs like mild swelling, changes in urine color, or intermittent fatigue are easy to dismiss, mistakenly attributed to stress, poor sleep, or aging, rather than potential renal issues.
High blood pressure is both a cause and effect of kidney dysfunction. Persistent hypertension strains glomeruli, the filtering units of the kidneys, leading to progressive loss of filtration capacity over time if left unmanaged.
Similarly, uncontrolled blood sugar in diabetes can damage delicate renal vessels. Even minor fluctuations sustained over months create cumulative harm, emphasizing the importance of consistent monitoring and lifestyle management.
Inflammation from chronic conditions, infections, or autoimmune disorders adds additional burden. The kidneys filter inflammatory byproducts, and ongoing immune activation accelerates tissue damage and scarring in renal structures.
Understanding kidney function highlights the interconnectedness of body systems. Poor renal health affects cardiovascular stability, bone density, red blood cell production, and fluid balance, demonstrating that kidney care protects overall wellbeing.
Dietary choices matter profoundly. Emphasizing fresh fruits, vegetables, lean proteins, and whole grains supports kidney function while reducing the workload imposed by excessive salt, processed sugar, and unhealthy fats.
Exercise complements diet by enhancing circulation, reducing blood pressure, and improving insulin sensitivity. Regular activity indirectly eases renal burden by supporting cardiovascular and metabolic systems that the kidneys depend upon.
Routine medical checkups are crucial. Blood tests for creatinine and estimated glomerular filtration rate (eGFR), urine analysis for protein, and blood pressure monitoring can detect early kidney stress, allowing timely interventions.
Kidney disease is often classified as chronic (CKD), reflecting its slow, progressive nature. Early intervention can prevent further deterioration, emphasizing prevention over reactive treatment after significant damage occurs.
Awareness is key. Many individuals do not consider kidney health until a major problem arises. Education about risk factors and early symptoms can dramatically improve outcomes for populations at risk.
Hydration should be balanced—not excessive, but sufficient to maintain optimal filtration. Experts generally recommend about 1.5–2 liters daily, adjusted for activity level, climate, and individual health conditions.
Medication use deserves caution. Over-the-counter drugs are not inherently safe for kidneys, and dosages, frequency, and duration should always follow medical guidance to minimize cumulative renal stress.
Chronic conditions like diabetes, hypertension, and obesity disproportionately affect kidney health. Managing these conditions through lifestyle, medication, and regular monitoring reduces strain and preserves long-term renal function.
The kidneys’ contribution to endocrine function is often overlooked. Hormones regulating blood pressure and red blood cell production originate here, demonstrating that renal health underpins vital processes beyond waste removal.
Toxin exposure through the environment, certain chemicals, and lifestyle choices can amplify renal strain. Limiting contact with nephrotoxic substances and maintaining a healthy lifestyle reduces cumulative risk.
Kidney stones, though sometimes acute, can also signal chronic stress. Excess salt, low fluid intake, or metabolic imbalances promote crystallization, causing pain and potential obstruction if unaddressed.
Silent kidney damage is frequently reversible in early stages. Lifestyle modifications, dietary changes, and medical management can restore function or prevent further decline, highlighting the importance of early detection.
Even subtle urinary changes warrant attention. Increased frequency, foamy urine, or unexpected color shifts are often dismissed but may indicate underlying renal issues requiring professional evaluation.
Sleep quality also impacts kidney health. Poor sleep contributes to metabolic dysregulation, elevated stress hormones, and increased blood pressure, all of which can silently burden renal function over time.
Stress management techniques—including mindfulness, meditation, and physical activity—reduce systemic inflammation and blood pressure fluctuations, indirectly protecting renal filtration and long-term kidney resilience.
Inflammatory markers in blood, such as C-reactive protein (CRP), correlate with kidney stress. Monitoring these markers alongside kidney-specific tests can guide proactive interventions.
Supportive supplements may help, but caution is advised. Overuse of herbal remedies or excessive vitamins can be nephrotoxic, emphasizing that even natural substances require careful consideration.
Kidney health is intimately tied to heart health. Reduced renal function elevates cardiovascular risk through fluid imbalance, hypertension, and electrolyte disturbances, highlighting the systemic consequences of neglecting renal care.
Mindful nutrition is a powerful tool. Limiting processed foods, added sugars, and excessive sodium reduces renal workload, prevents fluid retention, and maintains healthy blood pressure levels essential for kidney longevity.
Family history is a significant factor. Individuals with relatives affected by kidney disease should be especially vigilant, as genetic predispositions can interact with lifestyle factors to accelerate decline.
Screening programs in high-risk populations improve outcomes. Early identification allows for interventions, including medication adjustments, dietary changes, and lifestyle modifications to slow progression before irreversible damage occurs.
Psychological wellbeing also plays a role. Chronic stress, depression, and anxiety influence hormonal balance, blood pressure, and inflammation, demonstrating that mental health care is a silent yet essential component of kidney protection.
Patient education empowers proactive behavior. Understanding risk factors, early signs, and preventive strategies ensures individuals can maintain renal function, avoiding the common scenario where damage is advanced before detection.
Community and healthcare support amplify individual efforts. Access to screening, counseling, and professional guidance helps people implement sustainable lifestyle adjustments to protect kidney health effectively.
Hydration, nutrition, physical activity, stress management, and routine medical care form the foundation of kidney preservation. Neglecting any element increases the cumulative burden on these vital organs.
Kidneys exemplify quiet dedication. Unlike organs that signal distress loudly, they continue functioning under strain, often masking serious injury, which underscores the value of preventive care over reactive treatment.
Even minor adjustments—reducing processed food, increasing daily water intake, monitoring blood pressure—can substantially reduce the kidneys’ workload and preserve their capacity over decades.
Medical intervention may include controlling hypertension with ACE inhibitors or ARBs, managing blood sugar in diabetes, or prescribing medications to reduce proteinuria, all aimed at slowing renal decline.
Understanding kidney function provides perspective on overall health. Protecting these organs safeguards multiple systems, including cardiovascular, hematologic, and endocrine, making renal care central to comprehensive wellness.
Ultimately, kidney care is a long-term investment. The effort may seem subtle or unnoticed, but it prevents profound consequences and supports energy, resilience, and vitality well into later life.
Respecting the kidneys illustrates a broader principle: what works quietly is often the most essential. Attention, discipline, and preventive measures honor these hidden functions, preserving health before crises emerge.
Wise management begins before symptoms appear. Regular checkups, laboratory tests, and mindful lifestyle choices maintain renal health, reduce the risk of chronic kidney disease, and ensure these essential organs continue their silent work faithfully.
Protecting kidney health is a daily responsibility. Awareness, proactive care, and consistent healthy habits ensure the kidneys continue to function optimally, safeguarding life’s essential processes for years to come.